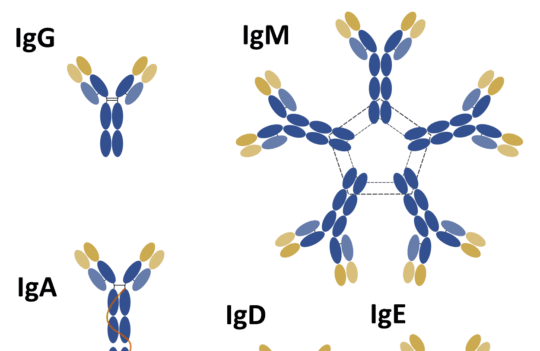
 Antibody production
Antibody production
Antibody therapeutics in clinical trials for the treatment of COVID-19
The race for the repurposing and development of treatments for COVID-19 continues amidst conflicting data on the new strain of coronavirus. Due to the shorter developmental times in comparison to new drugs, repurposed antibody therapeutics are one of the major players in clinical trials aiming to arrest the progression of the on-going pandemic. Which antibody treatments are currently leading the race to gain clinical approval for the treatment of COVID-19? What will the results of their clinical trials teach us about this new strain? Will these repurposed therapeutics be sufficient to mitigate the effects of the ongoing pandemic?
- Repurposing antibody therapeutics for the treatment of COVID-19
- Main antibodies in clinical trials for the treatment of COVID-19
- Antibodies targeting interleukin or interleukin receptors
- Tocilizumab and Sarilumab
- Clazakizumab and Siltuximab
- Ixekizumab in combination with antiviral drugs
- Antibodies targeting other biomarkers
- Adalimumab
- Bevacizumab
- Camrelizumab and PD-1 mAb
- Eculizumab
- Emapalumab in combination with Anakinra
- Meplazumab
- Concluding remarks
Repurposing antibody therapeutics for the treatment of COVID-19
Despite the record-numbers of papers and preprints published every day on COVID-19, it is surprising how little we know about this new virus. SARS-CoV-2, the emergent pathogen described in Wuhan, first interacts with our organism through the ACE2 receptor-enriched cells in our nose and throat.
As the virus enters the cells and takes over its machinery to produce multiple copies of itself, the infection spreads, often without any visible symptom. If our organism’s immune system fails to stop the infection at this point, the virus migrates to our respiratory tract and lungs often resulting in the development of acute respiratory distress syndrome (ARDS).
Many COVID-19 patients suffering from ARDS end up in ventilators, as the infection and the body’s exacerbated response to its presence cause devastating and often fatal lesions in the lungs, kidney, and other essential organs.
According to many researchers, we are still learning how this virus acts in our organism. For many patients, it is often unclear what causes these lesions. In some cases, fatal outcomes seem to be triggered by an intense inflammatory response known as cytokine storm. In other cases, abnormal blood clots or blood vessel constriction may precipitate mortality associated with the COVID-19 disease.
All these different symptoms have been contributing to a fragmented and often contradictory picture of the new respiratory illness. Treating one type of symptom may contribute to the degradation of other essential functions, for this reason, it is still hard to predict what type of treatment or drug will have the best possibilities of arresting the progress of the disease.
Researchers agree that, repurposed antibodies are helping us alleviate the most aggressive symptoms of the new disease. These repurposed drugs will buy precious time while we strive to develop urgently needed therapeutics and vaccines for COVID-19.
Main antibodies in clinical trials for the treatment of COVID-19
Antibodies targeting interleukin or interleukin receptors
Tocilizumab and Sarilumab
As of April 2020, there are at least 22 open clinical trials for Tocilizumab and 1 for Sarilumab. The former either alone or in combination with other antibodies (i.e. Pembrolizumab) or antiviral drugs (i.e. Anakinra), is leading the race for the treatment of COVID-19.
Tocilizumab is a humanized antibody obtained from mouse and Sarilumab is a fully human antibody. They were both designed to target the interleukin 6 receptor (IL-6R) and are currently approved for the treatment of rheumatoid arthritis, cytokine release syndrome (CRS), among others. Mortality in some COVID-19 patients seems to be associated with an intense CRS response, for this reason, many believe Tocilizumab or its analog Sarimumab may be the best antibody therapeutics for the mitigation the severe effects of this disease.
Clazakizumab and Siltuximab
Unlike the two abovementioned antibodies, these antibodies both target the interleukin-6 molecule. Clazakizumab is a humanized IgG1 molecule already approved for the treatment of rheumatoid arthritis, psoriatic arthritis, cancer, among other conditions. While Siltuximab is a mouse/human chimeric antibody approved by the FDA for the treatment of multicentric Castleman’s disease.
As of now, there are two open clinical trials to test the efficiency and safety of Clazakizumab (CHICTR2000030089 and NCT04348500) and one other trial to test Siltuximab (NCT04329650).
Ixekizumab in combination with antiviral drugs
Ixekizumab is a mouse humanized antibody targeting interleukin 17A (IL-17A), a major mediator of tissue inflammation in many autoimmune diseases. This IgG4 molecule has been previously approved for the treatment of psoriasis.
At the moment, there is one open clinical trial (CHICTR2000030703) that aims to test the efficiency and safety of this antibody in conjugation with antiviral drugs. This immunosuppressive therapy may attenuate the immune response to SARS-CoV-2 and thus reduce the extensive lung injuries observed in patients.
Antibodies targeting other biomarkers
Adalimumab
At the moment, there is a single clinical trial approved to evaluate the efficiency and safety of adalimumab in COVID-19 patients (CHICTR2000030089). The fully human monoclonal antibody targets the human tumor necrosis factor (TNFα) and has been approved to treat several autoimmune, ophthalmological, and inflammatory conditions.
SARS-CoV-2 enters the cells by binding to the ACE2 receptor, this mechanism enhances TNFα production, a key molecule in the inflammatory response. This mechanism is similar to the one observed for SARS-CoV, the causative agent of the respiratory pandemic of 2003. Previous studies with this strain suggested that the use of anti-TNFα antibodies could result not only in the inhibition of TNFα production but also in the reduction of ACE2 expression and shedding, thus decreasing the chances of infection with this new strain.
Bevacizumab
There are 3 clinical trials open for bevacizumab, a mouse humanized antibody, already approved for the treatment of several types of cancer and ophthalmologic diseases. It was designed to target the human vascular endothelial growth factor A (VEGF).
VEGF is considered as one of the most potent vascular permeability inducers and a key player in the development of ARDS, acute lung injury, and pulmonary edema (excess of fluids in the lungs). Recent studies showed high levels of VEGF in COVID-19 patients, suggesting that the use of bevacizumab may help to suppress the formation of pulmonary edema and reduce the mortality in the most severe cases of the disease.
Camrelizumab and PD-1 mAb
Both antibodies target receptors for programmed cell death protein 1 (PD-1). Camrelizumab is a humanized antibody that is currently being evaluated for the treatment of oncological disorders. On the contrary, very little is known about PD-1 mAb, except that it targets the same marker as Camrelizumab.
These treatments differ from the previous ones because instead of attempting to block the inflammatory response, they aim at reducing sepsis. Prior studies have suggested that targeting the excessive inflammatory response often fails to improve the survival of patients. PD-1 is a key mediator of T cell depletion in sepsis patients. For this reason, these antibodies may provide an important alternative to common anti-inflammatory drugs already being tested for the treatment of COVID-19.
Eculizumab
Eculizumab is a mouse humanized antibody targeting C5 (complement 5) and previously approved to treat several autoimmune and hematological conditions. At the moment, there is a single clinical trial (NCT04288713) designed to test the efficiency of this antibody against COVID-19 pneumonia.
Prior studies with the 2003 pandemic strain of coronavirus – SARS-CoV – revealed that the infection led to the activation of the complement cascade in the lung. Moreover, the study revealed that complement activation played a crucial role in a systemic and aggressive immune response to this strain of the virus. For this reason, since the new strain shares many characteristics with the SARS-CoV, this treatment could potentially delay the development of ARDS in later stages of the disease.
Emapalumab in combination with Anakinra
Emapalumab is a fully human antibody targeting IFN-g (interferon-gamma) approved for the treatment of primary hemophagocytic lymphohistiocytosis. As of now, there is a single clinical trial approved to test the efficiency and safety of this antibody for the treatment of COVID-19.
IFNG, like interleukin ligand 6, as been shown to play a key role in the hyperinflammatory response to COVID-19. For this reason, researchers believe that this antibody in conjugation with the antiviral drug Anakinra may delay the onset of ARDS in patients suffering from the most severe effects of the disease.
Meplazumab
Meplazumab is a humanized antibody that binds CD147. Recently, researchers observed that this antibody could inhibit SARS-CoV-2 infections in vitro, presumably due to the virus interaction with the CD147 receptor. For this reason, this antibody, instead of treating the symptoms of the disease, could instead block the entry of the virus and thus help the body clear the infection.
There is a single clinical trial registered to test the efficiency and safety of this antibody (NCT04275245). The results of the clinical trial have been recently published as a preprint; they indicate that the majority of the 17 patients enrolled in the study recovered rapidly after treatment with Meplazumab. However, further studies are necessary to evaluate the large-scale effectiveness of this new antibody.
Concluding remarks
Repurposing antibody therapeutics is possibly the fastest way to mitigate the effects of the COVID-19 pandemic, but they will likely only alleviate the most aggressive symptoms of the disease and only prove to be effective for some specific cases. Unlike new drugs, that need to undergo extensive antibody engineering and preclinical tests for toxicity evaluation, these drugs can be directly tested on the treatment of COVID-19. At the moment, several antibodies, either alone or in combination with other antibodies or antiviral drugs, are being tested around the world.
The majority of these biotherapeutics targets interleukin or interleukin receptors, major players in the cytokine release syndrome (CRS) associated with fatal outcomes in other respiratory infections (e.g. influenza). Most of the other antibody therapeutics under evaluation are also anti-inflammatory drugs, except for Meplazumab that may be able to bind to CD147, a presumed SARS-CoV-2 cellular receptor, and PD-1 antibodies that aim at delaying the development of sepsis in COVID-19 patients.
The outcomes of these clinical trials may not only produce a suitable therapeutic drug for immediate treatment of COVID-19 but also provide a deeper understanding of how this virus acts and interacts with our organism. Nevertheless, one thing is clear, these anti-inflammatory drugs may not serve all patients severely affected by the disease. For this reason, it is still vital that we continue to develop treatments specific to SARS-CoV-2.
- Bian, H. et al. Meplazumab treats COVID-19 pneumonia: an open-labelled, concurrent controlled add-on clinical trial. medRxiv. doi: 10.1101/2020.03.21.20040691
- Global Coronavirus COVID-19 Clinical Trial Tracker. Available on https://www.covid19-trials.com/. Accessed on April 20, 2020
- Garg, M et al. Imbalance of the renin-angiotensin system may contribute to inflammation and fibrosis in IBD: a novel therapeutic target? Gut. 2019; pii: gutjnl-2019-318512. doi: 10.1136/gutjnl-2019-318512
- Gralinski, L.E. et al. Complement Activation Contributes to Severe Acute Respiratory Syndrome Coronavirus Pathogenesis. mBio. 2018; 9(5):pii: e01753-18. doi: 10.1128/mBio.01753-18.
- Mehta, P. et al. COVID-19: consider cytokine storm syndromes and immunosuppression. 2020; 395(10229):1033-1034. doi: 10.1016/S0140-6736(20)30628-0